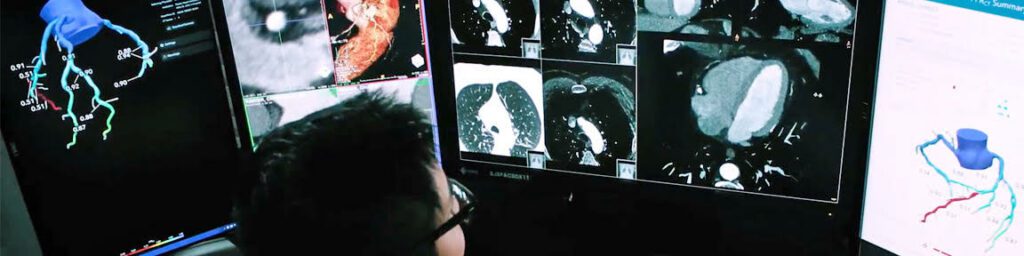
The New ACC/AHA Chest Pain Guidelines: Elevating Coronary CTA + FFRCT
All things come to him who waits – provided he knows what he is waiting for.
– Woodrow Wilson
For the first time in nearly a decade, the American College of Cardiology (ACC) and American Heart Association (AHA) have published new guidance that “provides recommendations and algorithms for clinicians to assess and diagnose chest pain in adult patients.” Behind this simply stated goal lie years of work by countless clinicians to identify evidence-based recommendations that will shape patient care for many years to come.
While some medical societal statements may feel overly complex or academic, practice guidelines are notable for laying out actionable pathways applicable to the patients seen in real-world clinical settings. The authors focus on contemporary imaging modalities for risk assessment and management planning in patients experiencing stable or acute chest discomfort. The new guidelines then further specify algorithms for patients with or without known CAD, and patients at different levels of overall risk.
A major shift in the long-awaited ACC / AHA guidelines is the elevated role of coronary CTA for the non-invasive assessment of patients with stable or acute chest pain. Coronary CTA is the only non-invasive testing modality given a Class 1 recommendation for patients with acute or stable chest pain supported by Level A quality of evidence. Furthermore, FFRCT is given a Class 2a recommendation across both acute and stable chest pain patient populations as it adds physiologic insight to the anatomic information provided by coronary CTA. Current dominant modalities such as stress imaging are classified lower than CTA, as Class 1 but with Level B quality of evidence.
The central reason for such clear recommendations in favor of coronary CTA in the new guidelines is overwhelming clinical data demonstrating that a CTA-driven pathway is
- Significantly better for patients, and
- Provides actionable information for clinicians.
For example, the guidelines indicate that coronary CTA is “effective for diagnosis of CAD, for risk stratification, and for guiding treatment decisions”(§5.1.3). In a similar fashion, the ability of FFRCT to help in “the diagnosis of vessel-specific ischemia and to guide decision-making regarding the use of coronary revascularization” (§4.1.2.1, §4.1.2.2, §5.1.3, §5.2.2) is highlighted throughout the guidelines. In contrast, stress imaging is described merely as “effective for diagnosis of myocardial ischemia and for estimating risk of MACE” (§5.1.3), without actionable information or connection to treatment guidance.
Finally, as the focus on chest pain management with medications becomes ever stronger, rather than immediate evaluation with invasive coronary angiography (ICA), it is worth noting that symptom persistence despite guideline directed medical therapy (GDMT) is required for Class 1 recommendation for ICA EXCEPT for when coronary CTA shows one of the following: “coronary CTA-defined ≥50% stenosis in the left main coronary artery, obstructive CAD with FFRCT ≤0.80, or severe stenosis (≥70%) in all 3 main vessels” (§5.2.1). Thus, FFRCT is recognized as a critical tool to aid physicians in determining which patients’ risk is such that ICA is warranted.
The anticipation that has preceded the release of the new ACC / AHA Chest Pain guidelines reflects how vital the need is for non-invasive testing that can help guide treatment decisions in today’s practice of cardiovascular care. Even before a global pandemic, clinicians were faced with the challenge of making better use of limited imaging equipment and interventional cath labs as patient numbers have been growing faster than capital resources at the majority of facilities. In this situation, many clinicians indicate that they can no longer rely on stress testing that often leads to layered testing or unnecessary invasive angiograms in more than 50% of the patients sent for ICA.
At a time when clinicians are increasingly asked to take bold action to improve health care delivery, the ACC and AHA have taken a significant step in elevating coronary CTA and FFRCT to steer clinicians towards a precise, patient-driven approach in the assessment and management of CAD.
— A perspective from HeartFlow Chief Medical Officer, Campbell Rogers, MD
Bio | LinkedIn





